FAQ
All you need to know about IVF Treatment
The team at Star Fertility Group is committed to the physical and emotional needs of our patients and the community. We understand that infertility can create a tremendous amount of stress, which is only intensified by uncertainty.
Here are a few of the questions we most commonly hear, and generally accepted.
Our support team is always on hand to offer advice or to put your mind at ease. Please do not hesitate to get in touch if there is something we have missed here. You should write in or request an appointment.
1.Why can't I get pregnant after 1 whole year of un-protected sex with my boyfriend / husband?
Well, it's not exactly your fault. Here's a look at the infertility rates :
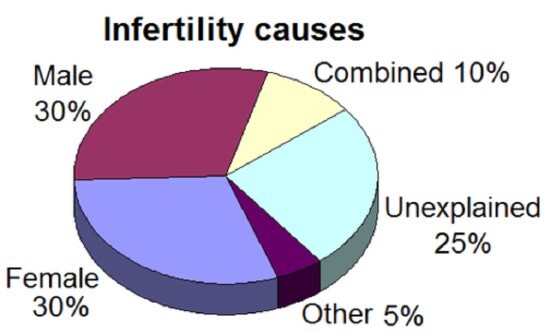
The best way to find out the cause is to get yourself checked by a fertility specialist or gynaecologist. Just call and make an appointment with them.
2. What are the causes of female infertility?
-
Blocked or damaged fallopian tubes
- Ovulatory problems
- Hormonal disorders
- Polycystic Ovary Syndrome, PCOS
- Endometrioses
- Being over 38, from which age fertility declines rapidly
- Medical conditions such as diabetes, epilepsy, and thyroid and bowel diseases
- Lifestyle factors such as stress, being overweight or underweight, alcohol misuse and smoking
- Environmental toxins including exposure to pesticides and lead
- Excessive physical or emotional stress that results in amenorrhea (absent periods)
3. What are the causes of male infertility?
Low number of sperm produced, or not at all (Azoospermia is a term used when there is a complete absence of sperm in the ejaculate)
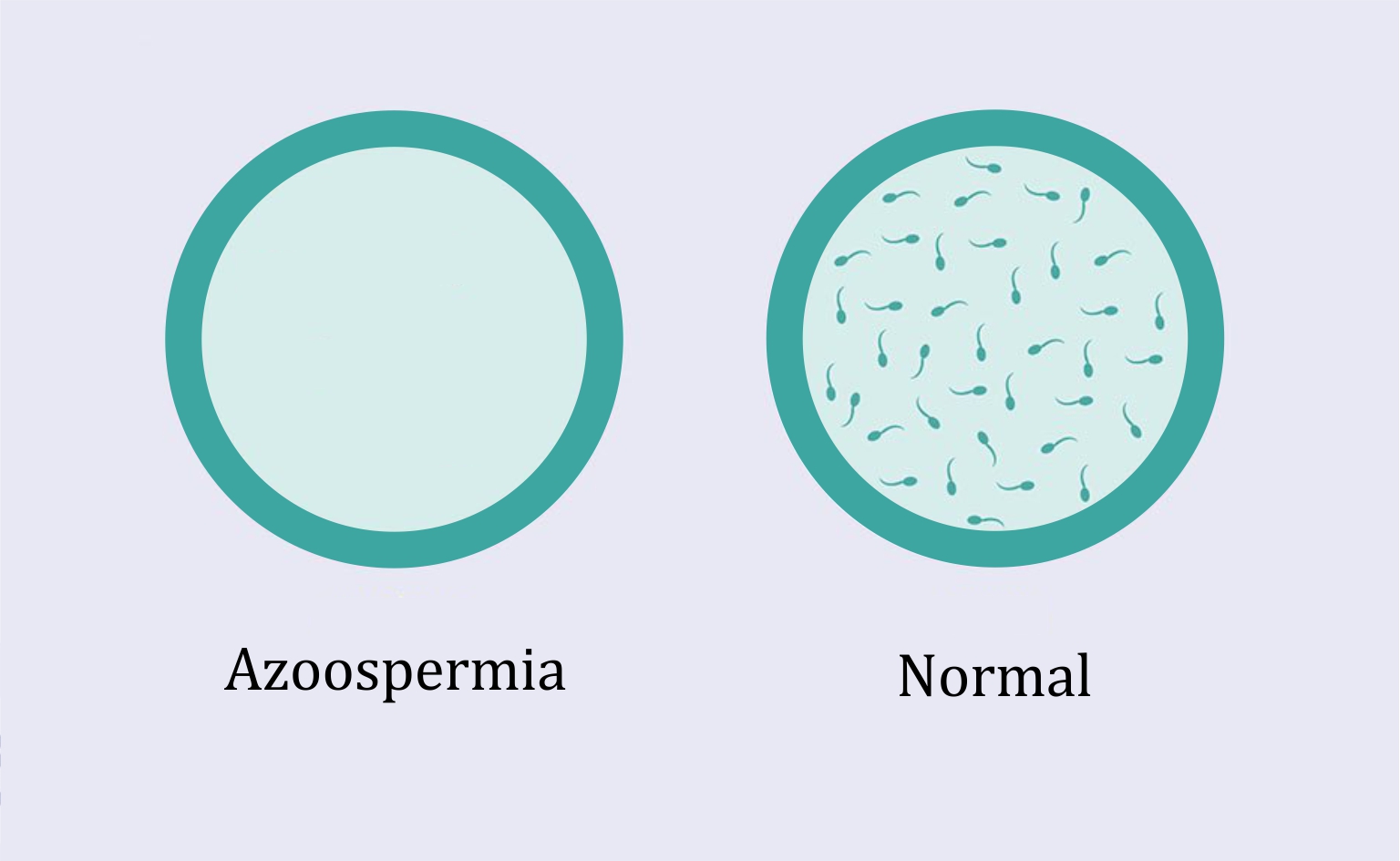
Azoospermia may be caused by:
-
Genetic abnormality
-
Failure of sperm production :
- Following a vasectomy
- Physical injury
Blood tests to investigate hormone levels may be required. A testicular biopsy may be required to determine the ability of the testicles to produce normal sperm.
-
Sperm being obstructed from ejaculation
-
Sperm that don't swim very well in the female reproductive system restricting its ability to reach and fertilise an egg
-
Oxidative stress resulting from injury, infection or smoking causing semen defects
-
Lifestyle factors such as stress, being overweight or underweight, alcohol misuse and smoking
-
Environmental toxins including exposure to pesticides and lead
4. How long should we continue trying to have a baby on our own before seeking help for fertility?
According to World Health Organization (WHO) on infertility definition, couple should seek fertility treatment after 12 months of unprotected intercourse, with the same partner, without resultant pregnancy.
5. How do I start?
Step 1 - Make an appointment for consultation session with our Fertility SpecialistStep 2 - Preliminary Investigations
Step 3 - Getting Started
Step 4 - Confirm treatment plan with your Fertility Specialist
Step 5 - Begin IVF Treatment
6. What are the preliminary investigations that me and my partner need to go through?
For Her
-
AMH
-
Vitamin D
-
Hysterosalpingogram
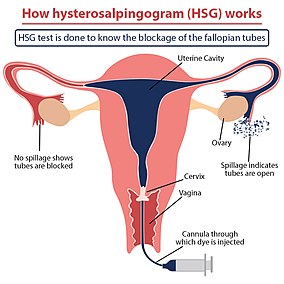
-
Ultrasound scan
For Him
-
Semen analysis
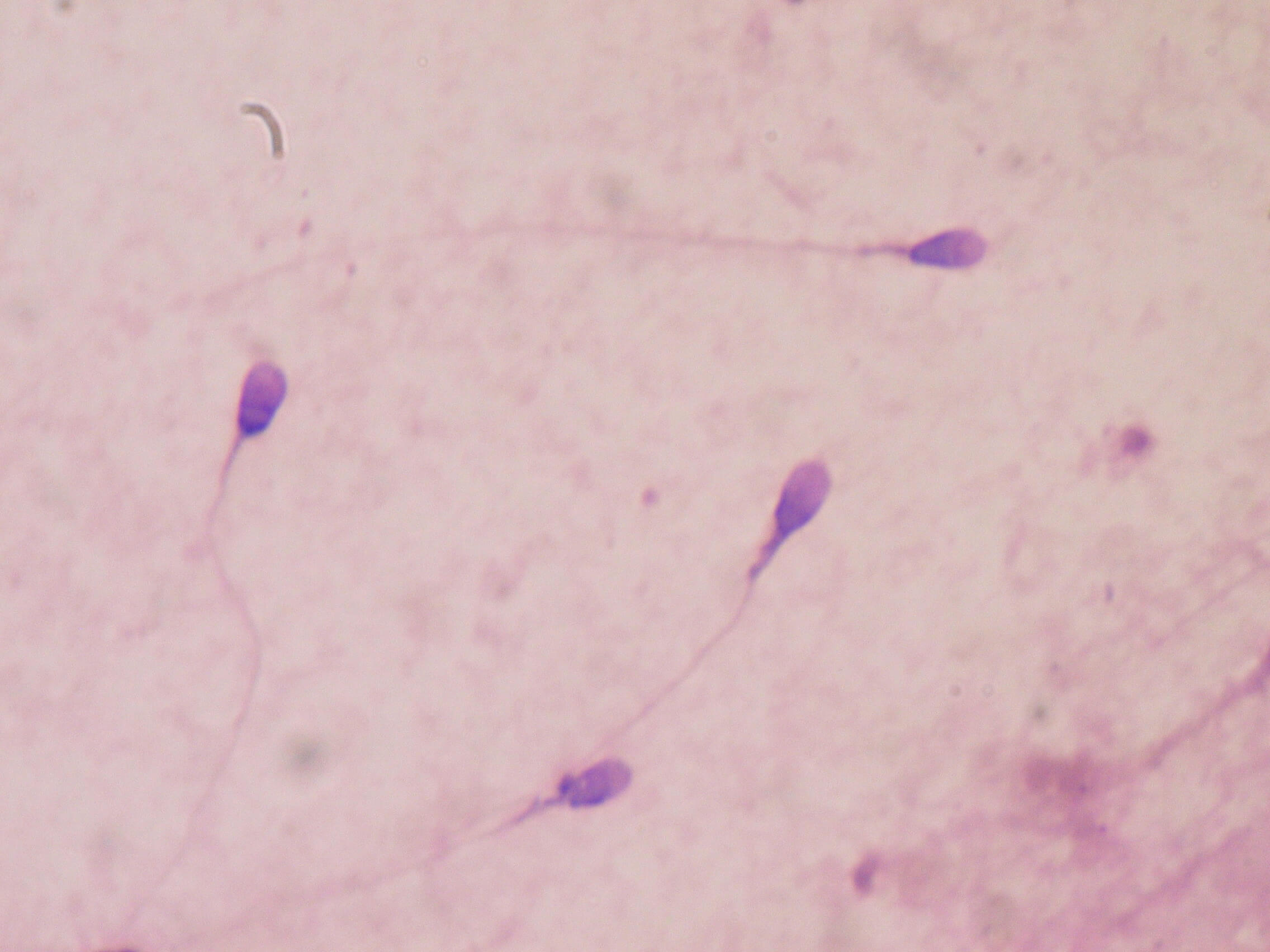
-
Blood test (if require as recommended by Fertility Specialist)
7. How much does fertility treatment cost? Will my insurance cover for my fertility treatment?
The cost of treatment depends on the options of treatment. Please contact Star Fertility Group for further information.
No insurance coverage for fertility treatment is available.
8. What about EPF withdrawal to fund fertility treatment?
The EPF allows all members to make withdrawal from your Account 2 for reimbursement to your fertility bill expenses for below treatment :
1. IVF Treatment
2. ICSI Treatment
3. IUI (Intrauterine insemination) Treatment
For further details of the withdrawal, kindly follow the below link:
https://www.kwsp.gov.my/en/member/withdrawals/partial/health#Fertility_Treatment
9. Is it painful to have the eggs retrieved? How long does an egg retrieval take?
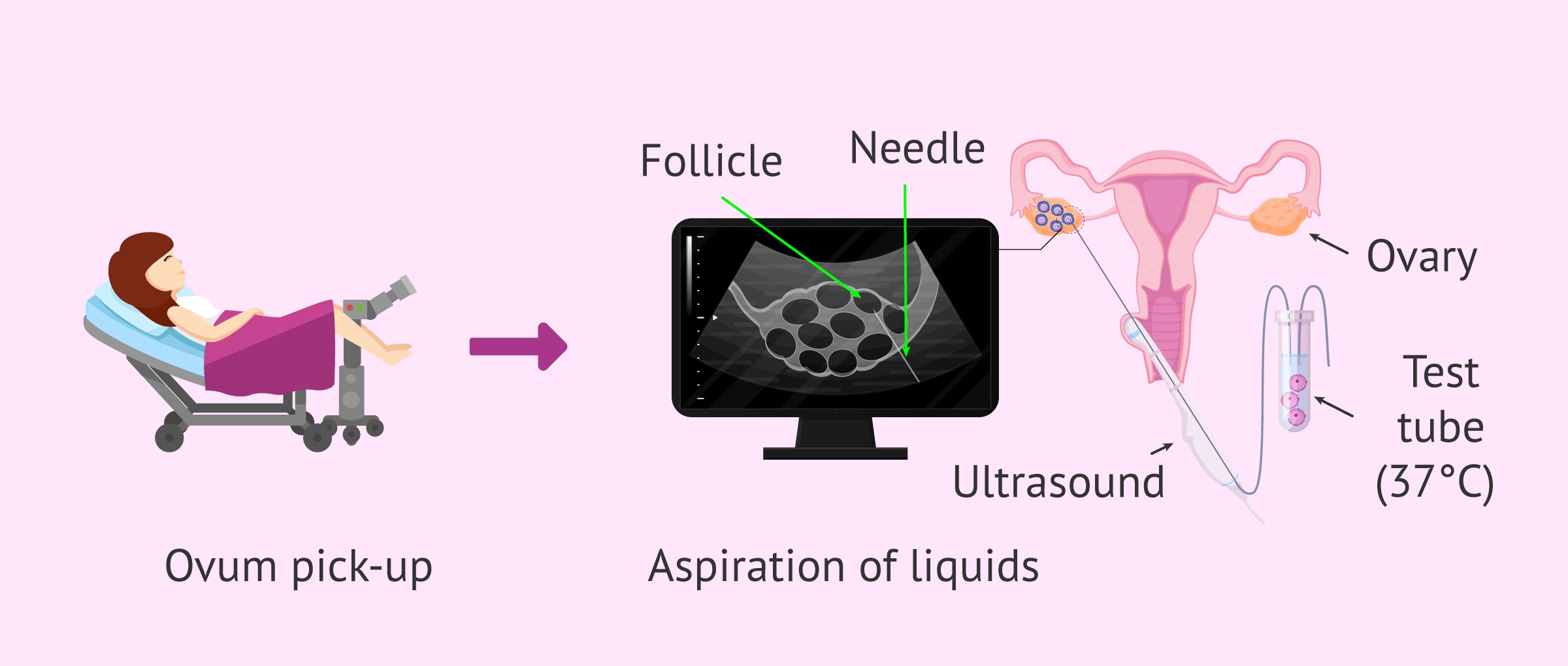
The egg retrieval (also known as Ovum Pick-Up procedure, or OPU), will be performed under sedation; our patients are asleep. The beauty of this approach is that you will feel absolutely nothing, remember absolutely nothing, and will have few of or none of the typical side effects of sedation such as nausea and vomiting. The OPU procedure lasts approximately 20 to 30 minutes. You will be discharged several hours after procedure within the day of OPU.
10. What is Intracytoplasmic Sperm Injection or ICSI?
For IVF treatment, two methods of fertilization are available:
1. Conventional In-Vitro Insemination (CIVI)
2. Intracytoplasmic Sperm Injection (ICSI)
CIVI, formerly known as conventional IVF, involved co-incubation of oocytes with sperm in culture dish with the goal to produce in-vitro fertilization, which mimic the natural way of fertilization in the women's reproductive tract, in which the sperm will have to penetrate the egg's wall (known as the zona) in order to reach the egg's cytoplasm to establish fertilization.
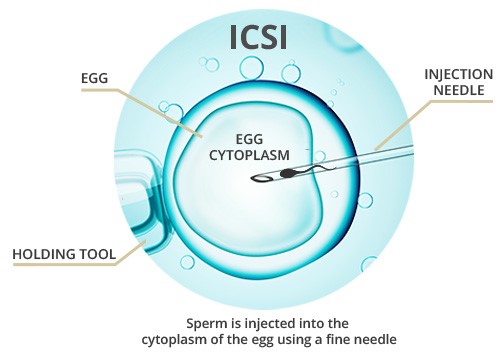
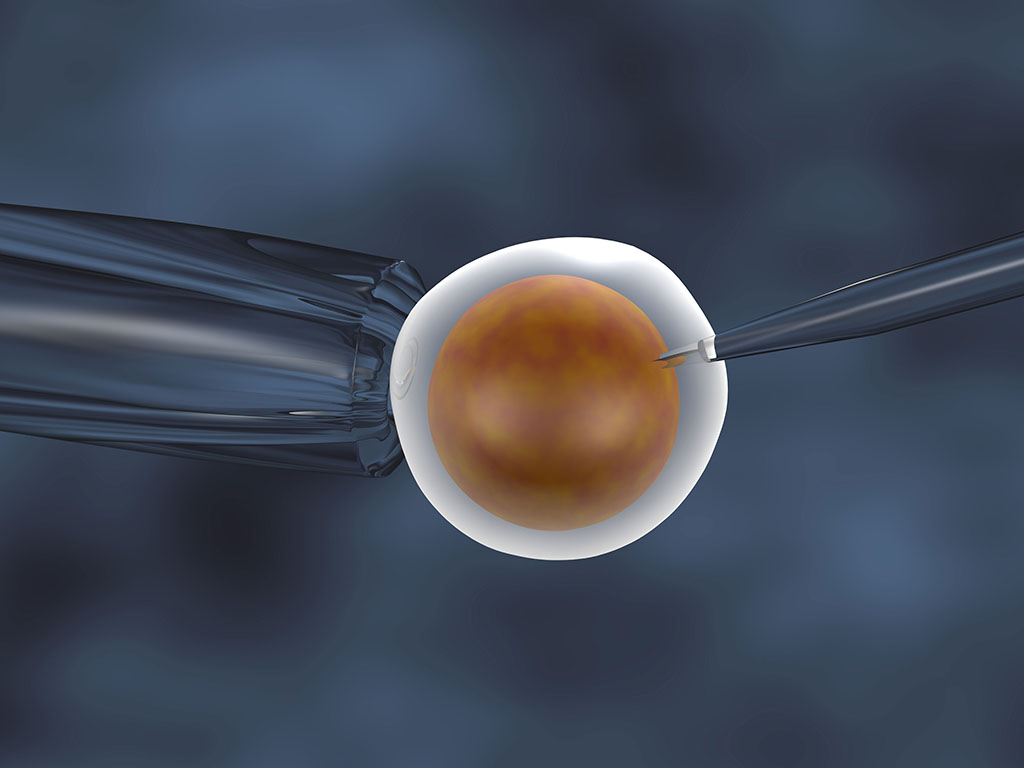
On the other hand, ICSI is a procedure in which a single spermatozoon is selected and injected directly into the mature oocyte cytoplasm by embryologist.
For both of the fertilization techniques, determination on the successful of fertilization (define by formation of pro-nuclei from both sperm and egg) can only be done on the next day after insemination.
11. What stage of embryo can be transferred in an attempt to established pregnancy in IVF treatment?
In general,
Day-1 Zygote,
Day-2 & Day-3 cleavage stage embryo,
Day-4 morula and
Day-5 or Day 6 blastocyst can be transferred.
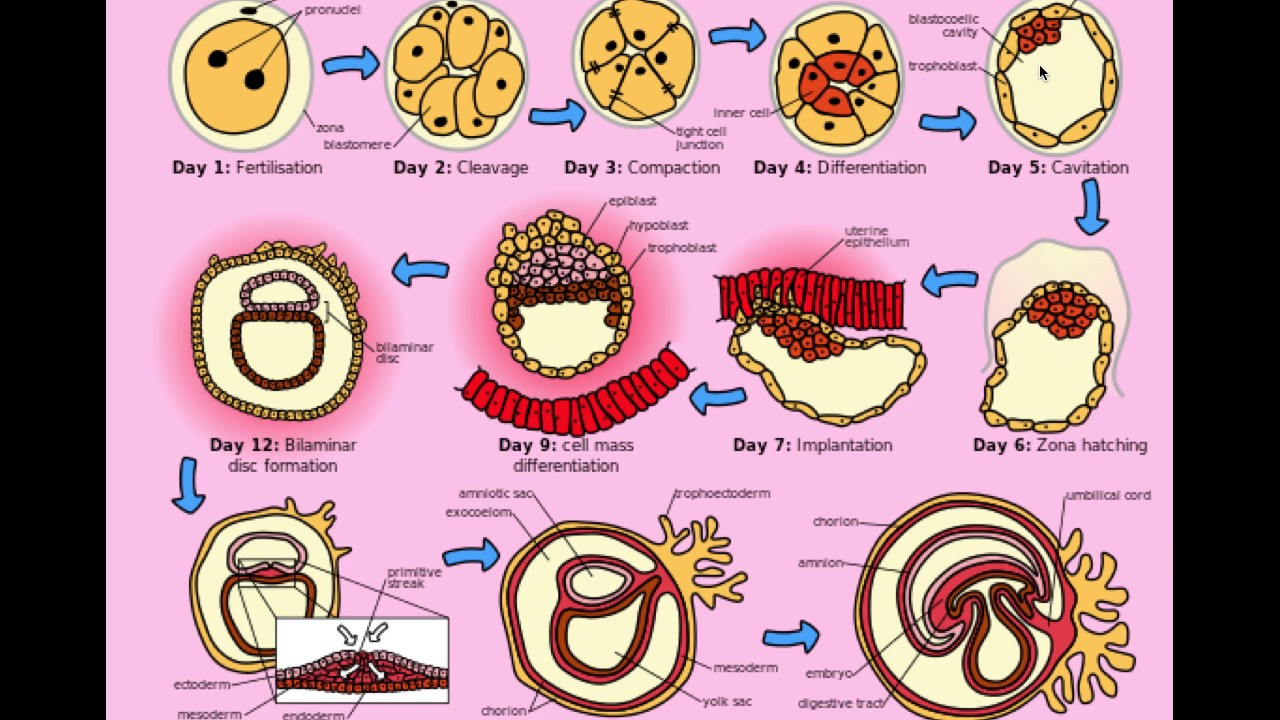
Day 1 - Fertilized Egg / Zygote
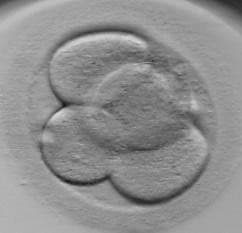
Day 2 - 4 Cells Stage Embryo
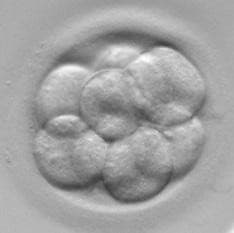
Day 3 - 8 Cells Stage Embryo
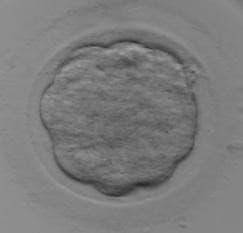
Day 4 - Compacting Morula
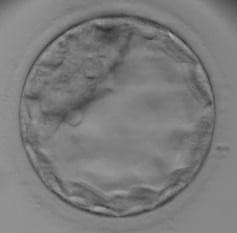
Day 5 / 6 - Blastocyst
However, it has been proven and clinically accepted that among all stages of embryos, blastocyst gave the highest chance of implantation compared to transfer of early stage embryo.
Reason for blastocyst transfer are:
-
Embryo selection play a crucial role in determining your chance of pregnancy. It is known that majority of the embryos are destined to arrest at the early stages of development, extended culture (or blastocyst culture) allows the embryologist to identify high potential embryo for implantation to transfer back into your uterus.
-
Transferring embryo at the blastocyst stage provides a better coordination between embryo and the uterus by putting the embryo back at the right stage (blastocyst) at the right place (uterus). Where else, early-stage embryo (which include zygote, cleavage stage embryo and morula), are mean to adapt to environment in Fallopian tube instead of uterus.
(* Please take note that during embryo transfer procedure, your doctor will place the embryo in the uterus and not the Fallopian tube.)
12. What are the chances to get conceived with IVF treatment?
The successful of IVF treatment is depending on several factors from both partners including age, weight and emotional stress. It is generally accepted that women's age play a crucial role in determining egg's quality, and eventually, fertility treatment outcomes.
13. How many embryos is suitable for transfer?
For every couples going through fertility treatment, it is understandable that main focus is to get pregnant and may think that having two or more embryos transferred to the womb could increase the chances to make that happen.
But, did you know that putting more than one embryo back in the womb could increase the health risk to both the mother and the babies? Twin or triplets babies might seem wonderful, but the reality could be much more complicated than what you can expect, the likelihood of your babies born prematurely is six times higher compare to a singleton pregnancy, which can lead to long-term health problems such as difficulty breathing, cerebral palsy and other physical and learning difficulties of your babies.
We encourage couple to transfer not more than two embryos, preferable single embryo transfer for women aged below 35 years old to reduce the risk of multiple pregnancy.
14. What is multiple pregnancy and what are the risks?
Multiple pregnancy, usually referred to as multiple gestation, is one in which more than one fetus develops simultaneously in the mother's womb. Multiple pregnancy is more difficult and poses more health risks than single pregnancy. Premature birth is greater with each additional fetus.
'One at a Time' Concept
Multiple pregnancy in fertility treatment can be reduced with elective Single Embryo Transfer (eSET) - having one embryo transfer back in the womb. The remaining good quality embryo (s) can be frozen for future use in later cycle.
Complications of Multiple Pregnancy
Multiple gestations can have many of the following complications:
-
Increased rate of spontaneous abortion
-
Two to three times greater risk of developing severe hypertension or preeclampsia (increased blood pressure)
-
Maternal anemia due to increased fetal demands
-
Premature rupture of membranes (bag of water)
-
Incompetent cervix (cervix opens due to pressure)
-
Intrauterine growth restriction of one or more fetuses
-
Preterm labor due to overstretched uterus
-
Abnormal fetal presentations
-
Need for cesarean section
-
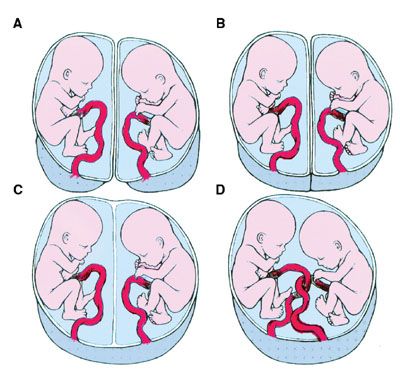
Rare complications with twins, such as twin-to-twin-transfusion syndrome (one fetus receives more nutrients than the other due to more blood vessels perfusing one baby)
-
Conjoined twins
-
Postpartum hemorrhage
15. What is Freeze-all cycle?
The freeze-all strategy has emerged as an alternative to fresh embryo transfer (ET) during IVF treatment.
Freeze-all cycles involve creating embryos using IVF treatment and then freezing all of the available embryo so fresh embryo transfer is performed. The frozen embryos can be thawed on the next cycle or few cycles later and transferred to the woman's womb as part of a frozen embryo transfer (FET) cycle.
16. Why frozen-thawed embryo transfer give higher pregnancy rate compared to fresh transfer?
Controlled Ovarian Stimulation during IVF treatment caused suboptimal uterine environment that negatively impact embryo implantation, and thus clinical pregnancy outcome.
Conversely, frozen-thawed embryo transfer cycle allowed sufficient period of rest from hormonal stress due to controlled ovarian stimulation during IVF, thus, cultivates better environmental condition within the uterus during embryo transfer, and enhance implantation with subsequent higher clinical pregnancy outcome compared to fresh transfer.
17. How soon after IVF will I be able to know my pregnancy status?
A pregnancy blood test (βhCG) is usually done 12-14 days after embryo transfer, while a confirmation of clinical pregnancy test via ultrasound scan will be done 19-21 days post embryo transfer.
18. How long of a wait is recommended between a failed IVF cycle and trying again?
We would recommend at least one full menstrual cycle of waiting before undergoing IVF a second time. We know that it can take up to 6 weeks for inflammation to resolve; therefore, it is reasonable to wait a similar amount of time before restarting the process.
19. What are other risks related to fertility treatment (apart from multiple pregnancy)?
Fertility treatments are generally very safe. However, as with any medical treatments or surgical procedure, fertility treatment carries some risks to be aware of, which range from mild to discomfort to more serious conditions. Other risks, of which some are not yet fully understood, relate to the children born as a result of the treatment.
-
Reaction to fertility hormones
-
Ovarian Hyper-Stimulation Syndrome (OHSS)
-
Adnexal Torsion (Ovarian Twisting)
-
Complications from Egg-retrieval Procedure
-
Ectopic Pregnancy
Reaction to fertility hormones
You might develop a mild reaction to fertility drug during IVF cycle which include:
-
Hot flushes
-
Feeling down, irritable or mood swing
-
Headaches
-
Restlessness
Talk to your fertility specialist if the intensity of the reaction gets worse, she may be able to adjust your dosage or switch to another drug.
Occasionally, the side effects of fertility drugs could be serious. We advise you to contact your fertility clinic directly if you notice:
-
Allergic reaction - these include difficulty in breathing and tightness in your chest
-
The symptom of severe ovarian hyperstimulation (OHSS)
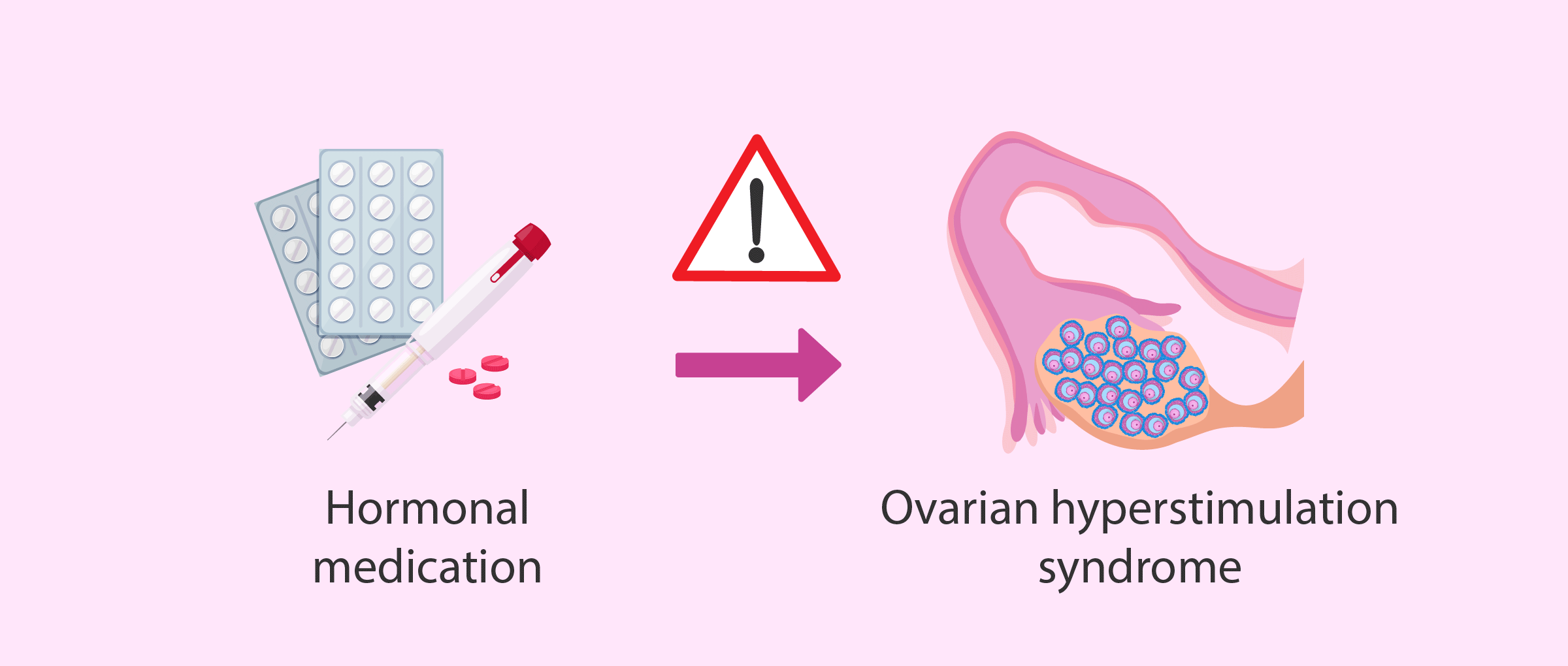
Ovarian Hyper-Stimulation Syndrome (OHSS)
OHSS occurs due to over reaction to fertility drug use in egg triggering, known as hCG trigger in IVF cycle. OHSS is characterized by enlargement of ovaries with presence of multiple corpus luteum cysts and shift of fluid into the extravascular space of abdominal cavity.
The chances of OHSS increase in women with:
-
Polycystic ovarian syndrome
-
Young age
-
Low body weight
-
Previous episodes of OHSS
-
High number of follicles
OHSS can be classified as mild, moderate, or severe according to the degree of symptoms which include abdominal distention, ovarian enlargement, respiratory, hemodynamic, and metabolic complications.
The symptoms of OHSS usually develop during the week after egg retrieval. Most cases of OHSS are mild and without any serious or prolong complication (usually lasts within a week or two). In some cases, your fertility specialist might consider delaying the embryo transfer by freezing the embryo and transfer at a later date. Occasionally, in rare severe cases, OHSS can be life threatening.
It has been proven that the risk of OHSS can be reduced by using GnRH Agonist triggering during IVF cycle. Consult the fertility specialist on the treatment regime associating with OHSS. Star Fertility Group takes into consideration of the risks and safety of OHSS seriously, and as a result, GnRH Agonist triggering is applied as a strategy to reduce your risk of developing OHSS.
Adnexal Torsion (Ovarian Twisting)
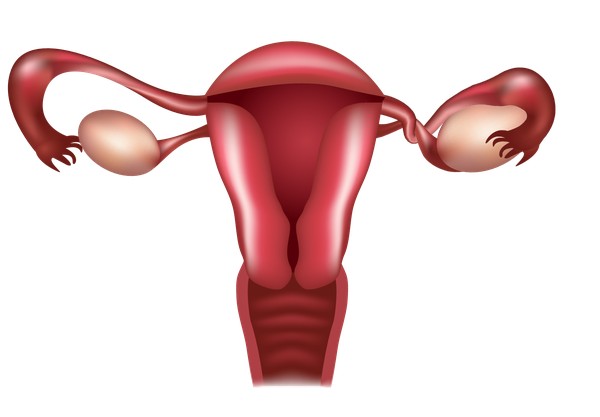
The term refers to when the stimulated ovary twists on itself, due to high number of follicles in the ovary, cutting off its own blood supplies. The overall risk is 0.2%. In a normal condition, the ovary is meant to carry only one mature follicle, however, due to stimulation in IVF cycle, the number of mature follicles increase, causing the ovary to become heavier and lead to twisting. Treatment is surgery to untwist the ovary and even removing it sometimes.
Complications from Egg-Retrieval Procedure
Egg retrieval or ovum pick-up (OPU), is a medical procedure to surgically remove eggs from a woman's ovaries transvaginally for IVF purpose.
Common complication post OPU includes:
-
Vaginal bleeding/spotting
-
Mild bloating
-
Mild cramping
-
Breast tenderness due to high oestrogen levels
-
Constipation
-
In rare occasion, pelvic infection might occur
OPU is a simple procedure; you will be allowed to go home several hours after completion of procedure with some antibiotics to prevent infection.
Ectopic Pregnancy
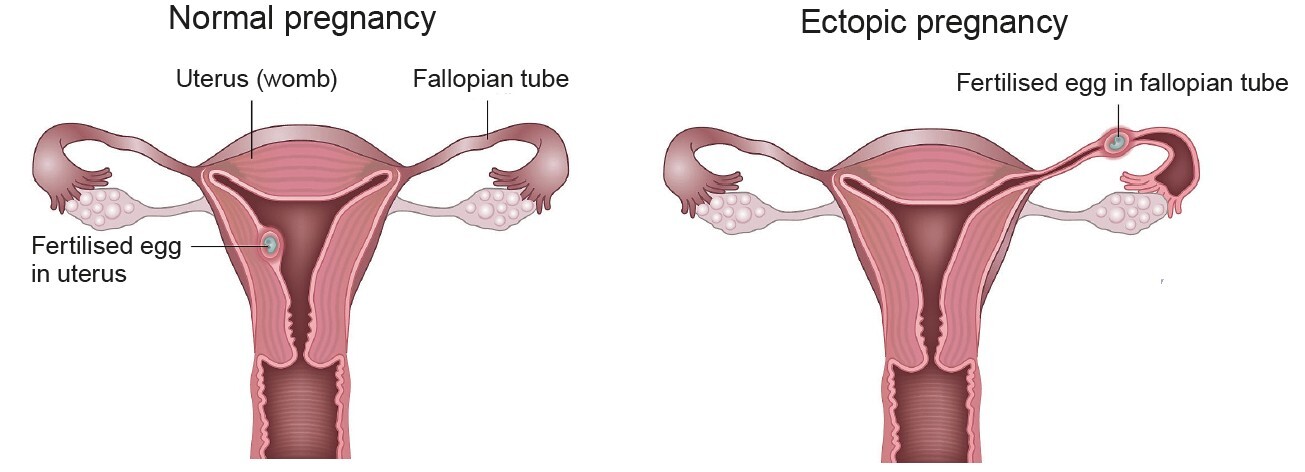
Ectopic pregnancy happens when the fertilised egg implants outside the uterus, usually in a fallopian tube. The incidence of ectopic pregnancy seems higher with IVF treatment, especially if you already have problems affecting your fallopian tube. However, it has been proven that blastocyst transfer is associated with lower risk of ectopic pregnancy compare to cleavage stage transfer (Day 2 or Day 3 transfer) in IVF treatment.
The symptoms of ectopic pregnancy may include:
-
One-sided low abdominal pain
-
Vaginal bleeding
-
Dark brown vaginal discharge
The pain intensifies as the pregnancy progresses. The major risk of ectopic pregnancy is rupture of the fallopian tube causing internal bleeding. You should talk to your doctor if you experience sharp abdominal cramp or vaginal bleeding in early pregnancy.
