Blog Template Not Full Width

When an embryo grows, it will multiply from 2, 4, 6, 8 cells until it becomes a blastocyst.
A blastocyst is a human embryo that has reached about 5 - 6 days after fertilization.
The embryo must reach this stage before it can hatch and implant itself into the lining of the uterus.
When the eggs are harvested and fertilized, the embryos that reach blastocyst stage can undergo PGT-A.
The PGT-A technique will take part of the cells from a blastocyst to test for any genetic abnormalities.
Day 5 biopsy is highly recommended, however, Day 3 biopsy is also possible especially when you are planning for fresh embryo transfer.
The procedure requires the use of laser to cut out a sample of the cells which will be sent for genetic testing by a genetic lab.
Poor quality embryos will not be able to withstand the cutting process as only good quality embryos will.
The genetic test results will be available within a month under normal circumstances.
However, express PGT-A results can be obtained but with a higher price.
PGT-A is considered the gold standard when it comes to genetic testing to detect for genetic abnormalities in embryos.
For instance, all the embryos may look normal under a powerful microscope.
But with genetic testing, it is able to detect if the embryo has any pre-existing genetic conditions whereby the results are made known to couples for them to decide whether to proceed with IVF or not.
The objective is to provide the best option for parents to choose.
PGT-A is also known as Pre-Implantation Genetic Screening (PGS).
Call or whatsapp our Penang IVF Centre to find out more about PGT-A option for your fertility treatment journey.

Understanding The Chromosomal Makeup Of Embryos
Each cell in the human body contains packages of genes called chromosomes.
Normal cells have 46 chromosomes arranged in 23 pairs (half from each parent).
Females have two X chromosomes, and males have one X and one Y chromosome in all their cells.
Embryos are called euploid if they have
the right number of chromosomes and aneuploid if they have extra or
missing chromosomes.
An aneuploid embryo is unlikely to implant and if it does implant, there is a high risk of miscarriage or serious health problems if a baby is born.
How is PGT-A done?
PGT-A adds one extra step to the IVF process. Here are the steps:
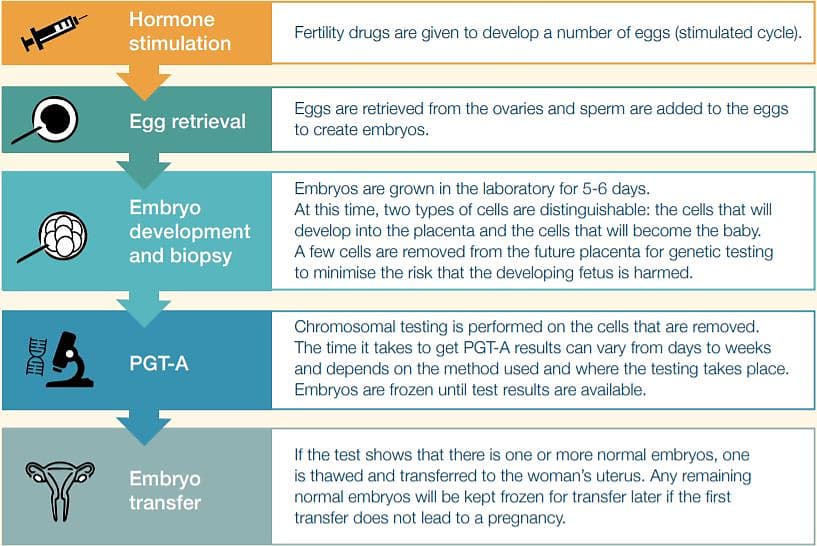
Advantages and disadvantages of PGT-A
It is important to know that PGT-A does not guarantee the birth of a healthy baby.
Women who become pregnant are advised to undergo prenatal testing (e.g. DNA testing or chorionic villus sampling) to confirm PGT-A results.
Here are some of the advantages and disadvantages of PGT-A.
Please note : You will be able to know the sex of your baby through PGT-A testing. However, sex selection is not allowed.
The embryologist and fertility specialist will suggest to you which is the embryo to transfer based on the PGT-A report.
Advantages of PGT-A
• PGT-A reduces the risk of having a child with a chromosomal abnormality.
• For women who have had unexplained miscarriages or who are 35 years and above, PGT-A can reduce the risk of future miscarriages.
• PGT-A can reduce the risk of having to make difficult decisions about whether to terminate or continue a pregnancy where the fetus has a chromosomal abnormality.
• For women over the age of 36, PGT-A can reduce the risk of miscarriage and the number of embryo transfers to achieve a pregnancy.
Disadvantages of PGT-A
• PGT-A does not increase the overall chance of having a baby.
• PGT-A is expensive and is in addition to the costs of IVF.
• Embryos may not survive the biopsy procedure.
• Due to technical challenges, there is a small chance that the test results may not reflect the true health of the embryo.
• Some embryos have a mixture of normal and abnormal cells. This is called mosaicism.
• Sometimes no embryo is suitable for transfer. Your embryologist will discuss your results and best options with you.
• Embryos may not survive the thawing process.
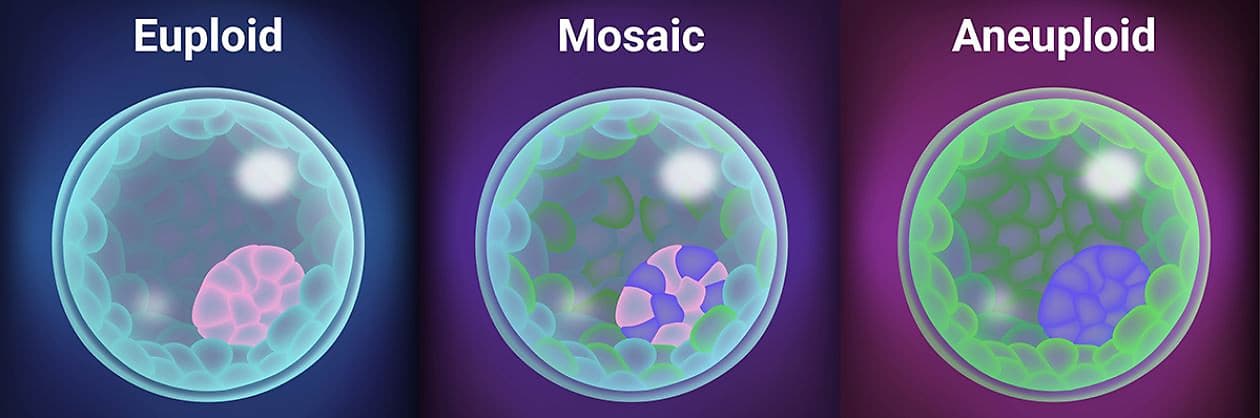
Euploid - correct number of chromosomes and genetically the best embryos to transfer with the highest chance of pregnancy success
Mosaic - an in between result where some cells in the test are euploid and some cells are aneuploid from an embryo which has some chance of success but typically less than euploid embryos
Aneuploid - incorrect number of chromosomes and an embryo which studies have shown have an almost 0% chance of success
